Healthcare System Essay on Germany
-
Osman Sirin
- December 17, 2022

Healthcare System in Germany and the Bismarck Model
Healthcare System Essay: Abstract
Healthcare systems have gained importance as a result of ongoing pandemics in 21st century. In this assignment, the healthcare system in Germany and the Bismarck Model have been analyzed. The paper also presents insights into the overview of the Bismarck Model, an overview of healthcare in Germany, health insurance in Germany, country health profile, health statistics, and a brief discussion. Upon analyzing the WHO and OECD data, along with many other sources, one can readily infer that Germany has a considerably reliable healthcare system and insurance system in terms of quality and quantity when compared with many other nations.
Introduction
Recent developments across the world have revealed probably the most significant system that is beyond politics, finance, and careers: the healthcare system across the world. The global combat against COVID-19 (Coronavirus) has presented insights into the health systems of various nations, as suggested by statistics worldwide (Hopman, 2020). That is, Germany is among the most effective countries in terms of treatment and handling the virus. Therefore, in this assignment, the healthcare system in Germany and the Bismarck model has been thoroughly examined. Statistics and examination have revealed that Germany has a considerably advanced healthcare system when compared with other European nations.
Overview of the Bismarck Model
Created by the Prussian chancellor, Otto von Bismarck, as a social welfare measure for German unification in 1883, the Bismarck Model is among the most known international health care systems across the world (Health Care Systems, 2019). The Bismarck Model is based on three core principles (Health Care Systems, 2019). Accordingly, the government is responsible for universal access to healthcare. Also, the smallest administrative units in society need to implement health policies properly. Moreover, elected authorities in term should organize negotiations to ensure the interests of medical care and medical care workers across the nation.
In the Bismarck Model, the insurance system is supported collectively by both employers and employees with the payroll taxes, called "sickness funds" (Nguyen et al., 2017). That is, these taxes are directly cut from the salary checks. Similarly, the United States also adopted the Bismarck-wise system. More specifically, "most Americans who are employed but not yet eligible for Medicare receive health insurance coverage from their employers as a benefit of employment"((Nguyen et al., 2017). Nevertheless, this approach is not as feasible as the German model because American employers can limit the list of health insurers.
The most significant advantage of the Bismarck Model is that it aims to cover every citizen, and it is not meant to make any profit. Instead, it is a humane approach to the well-being of all citizens. On the other hand, some may highlight the private hospitals and physicians in the countries where the Bismarck Model is applied. However, governments have strict audits over the insurance companies that are supposed to be non-profit. This way, one can readily infer that non-profit structure, along with fixed-price procedures, keep the costs at a low degree for citizens in the Bismarck Model.
Figure 1. Summary of Healthcare Models (Fan, 2018).
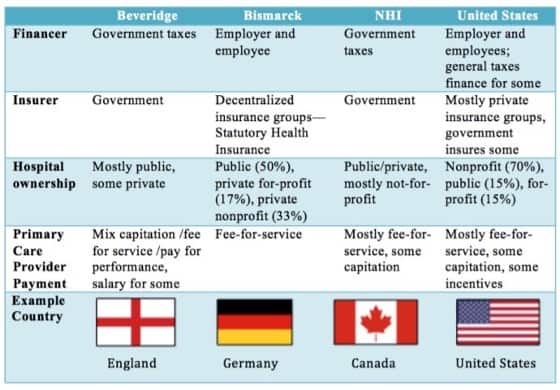
Along with certain disadvantages, one can readily list the advantages of the Bismarck Model. For instance, citizens do not face any issues regarding expensive health care bills or being uninsured. Also, the administrative costs of such a model are comparably lower than the US Model (Health Care Systems, 2019). Furthermore, citizens do not need to wait so much to receive primary care services. In other words, the Bismarck model is generally based on the well-being, functionality, and implementation of social health care services for all citizens in a country. Nevertheless, in the Bismarck Model, the mandatory taxes are comparably high to keep the health care services available and affordable for everyone. Also, when it comes to tertiary and secondary health care services, the waiting list can be long for patients when compared to other systems.
Overview of Healthcare in Germany
The German healthcare system is considered as the oldest in Europe, dating back to the 19th century. Today, the German Healthcare system is also considered among the best health care services in the world. The German healthcare system is funded “by statutory contributions, ensuring free healthcare service for all. Besides, one can also take out private health insurance [Private Krankenversicherung or PKV] to replace or top upstate cover [gesetzliche Krankenkasse or GKV] (A Guide to German Healtchare System, 2016). According to the 2018 Euro Health Consumer Index, Germany ranked as 12th among other health care systems across the world (A Guide to German Healtchare System, 2016). Although the country offers various types of treatments for citizens, the number of specialist hospitals negatively affected its score on the survey.
According to the German Healthcare System, all residents have direct access to healthcare services across the country. However, non-residents need to have private insurance in order to access health services. Similarly, temporary residents to the country should pay for the health services; however, they may ask for reimbursement later. The German Healthcare Systems also cover citizens from the European Economic Area [EEA], European Union [EU], and Switzerland with EHIC [European Health Insurance Card] (European Health Insurance Card, 2020).
Figure 3. Health Expenditure, 2016 (Healthcare Expenditure, 2018).
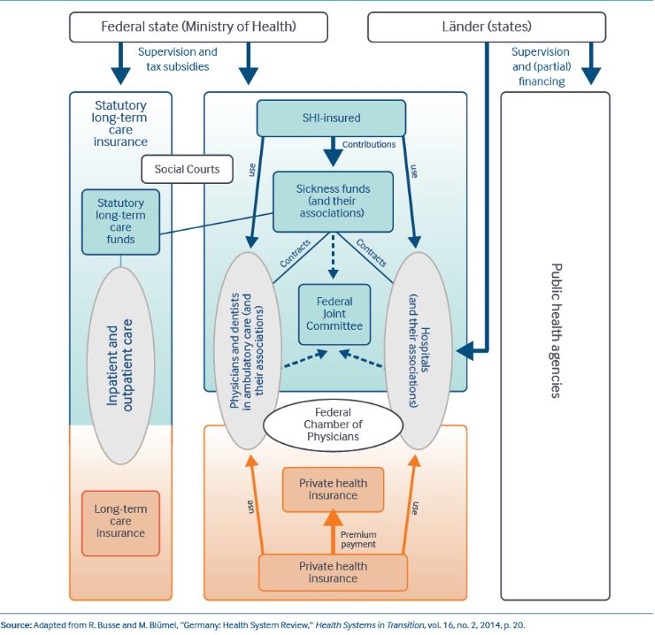
In terms of healthcare system costs, Germany is one of the biggest spenders on healthcare across the world, with 11.1% of annual GDP, as shown in Figure 2. Comparably, merely France and Switzerland seem to spend more than Germany. However, the majority of costs are covered by private and public insurance systems. That is, every resident needs to pay a fee of 10 to 15 EUR for their first medical visit every quarter, but this fee can be reclaimed for citizens with private health insurance (A Guide to German Healthcare System, 2016).
Figure 3. Health Expenditure, 2016 (Healthcare Expenditure, 2018).
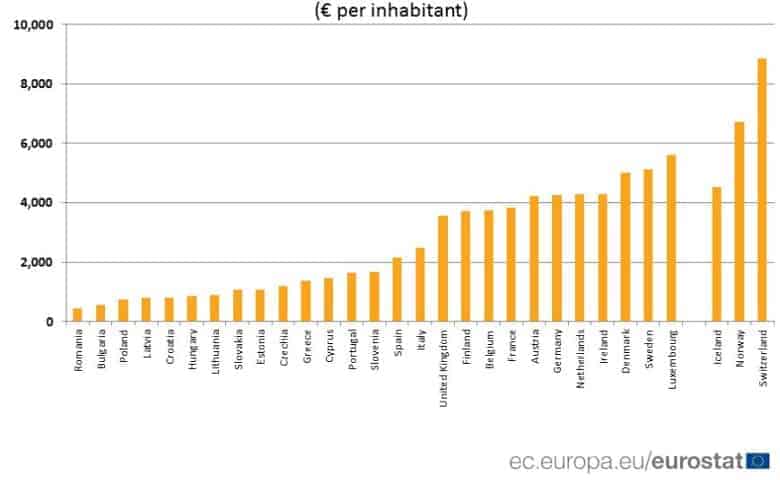
Health Insurance in Germany
Each employee, earning less than 57,600 EUR [broadly 4,800 EUR a month in 2017] a year, has to take part in the government health scheme—Gesetzliche Krankenversicherung or GKV—taking out health insurance as soon as the employee signed his/her work contract (A Guide to German Healthcare, 2016). The government health scheme is comprised of 110 Krankenkassen, which are non-profit organizations. They all need to charge the same rate of 14.6% of gross salary, up to a maximum of 4,350 EUR a month in 2017 (A Guide to German Healthcare, 2016).
The most advantageous function is that this amount is to be shared between employers and employees in the German health insurance system. However, one needs to stay in the same plan [scheme: Krankenkasse] for eighteen months. Then, a resident has the right to choose his/her own scheme. Also, the system seems to protect the employers a lot. That is, they are only eligible to pay for the insurance costs as long as they make more than 850 EUR per month. Moreover, hospital care [both in- and out- patient], primary care with registered doctors, and essential dental treatment are among the GKV coverage, and non-working dependents are also covered free within the insurance as long as they are registered to the same address (A Guide to German Healthcare, 2016). Expectedly, private rooms in hospitals, private doctor services, alternative treatments, contact lenses/glasses, and dental implants are not covered within the public insurance system provided by German administration.
Germany Health Statistics
According to OECD Library, “Germany spends more per person on health than other EU countries, providing a broad benefit basket, high level of service provision, and good access to healthcare" (Germany Country Health, 2019).
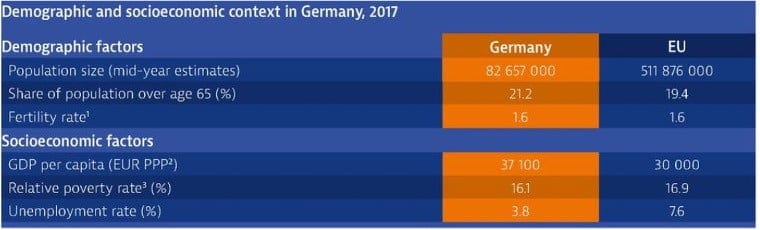
Figure 4. Demographic statistics of Germany, as of 2017 (OECD)
Figure 4 shows some statistics regarding the socioeconomic and healthcare of Germany. Accordingly, the share of the population over age 65 seems higher than the EU average. Similarly, GDP per capita is higher than the EU average of 30.000 EUR per year. However, the unemployment rate and relative poverty rate are lower when compared with the EU nations.
Performance of the Healthcare in Germany
Figure 6. Avoidable deaths from preventable and treatable causes, comparison with EU nations. (OECD, 2017).
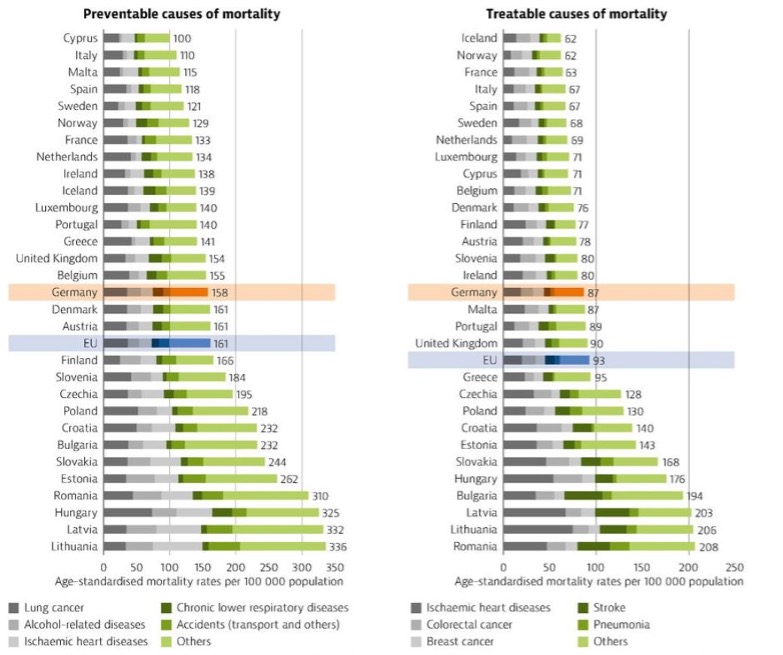
Although Germany tends to spend more on healthcare, Figure 6 shows that the EU average is better in terms of preventable causes of mortality and treatable causes of mortality.
Figure 7. Bed numbers and the average length of stay, compared with the EU average (OECD, 2017).
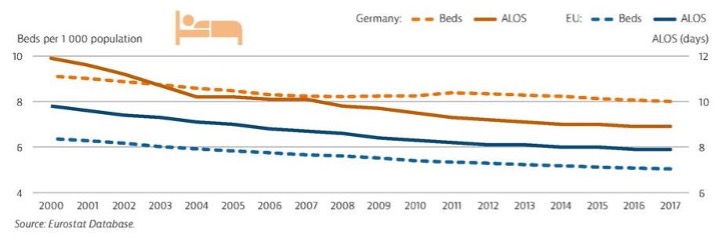
Figure 8. Most Germans have a doctor nearby, but there might be some problems in rural areas (OECD, 2017).

Figure 7 shows the statistics and distance of doctors in whole Germany. Accordingly, statistics have revealed that Germans have the least waiting line and reliable access a healthcare or doctor for an appointment (Germany Country Health, 2019).
Discussion and Conclusion
Upon analyzing the presented data above, one can observe that Germany has a considerably well-functioning system in terms of health insurance, healthcare system, doctor numbers, life expectancy, and medical assets. Accordingly, Germany spends much more money on the healthcare system than average EU countries. Also, the Bismarck approach to healthcare has already been proven effective. Moreover, the Bismarck model is known to prioritize the well-being of citizens, and a social state approach is ensured across Germany regarding the accessibility of healthcare. Overall, it is explicit that Germany has a definite advantage in terms of doctor frequency, bed numbers, average GDP, average money spent on health facilities, health insurance system, and socioeconomic factors. In conclusion, one can readily infer that Germany has a considerably reliable healthcare system and insurance system in terms of quality and quantity when compared with many other nations.
References
A Guide to the German Healthcare System. (2016, September 01). Retrieved May 19, 2020, from https://expatica.com/de/healthcare/healthcare-basics/german-healthcare-system-103359/
European Health Insurance Card. (2020). Retrieved May 19, 2020, from https://ec.europa.eu/social/main.jsp?catId=559
Fan, K. F. (2018). A Correlative Study on International Healthcare System Variables and Opioid Consumption Data. Oregon State University, 1-42. Retrieved May 19, 2020.
Germany: Country Health Profile, 2019: READ online. (2019). Retrieved May 23, 2020, from https://read.oecd-ilibrary.org/social-issues-migration-health/germany-country-health-profile-2019_36e21650-en
Health Care Expenditure in the EU. (2018). Retrieved May 19, 2020, from https://ec.europa.eu/eurostat/web/products-eurostat-news/-/DDN-20181129-2
Health Care Systems - Four Basic Models. (2019). Retrieved May 19, 2020.
Hopman, J. (2020, April 28). Managing COVID-19 in Low- and Middle-Income Countries. Retrieved May 19, 2020, from https://jamanetwork.com/journals/jama/article-abstract/2763372
Nguyen, A., Integrative Biology, & UC Berkeley. (2017, August 05). International Health Care Systems Part 3: The Bismarck Model. Retrieved May 19, 2020, from https://morningsignout.com/international-health-care-systems-part-3-the-bismarck-model/
Contents
Recently on Tamara Blog

Essay on Animal Farm by Orwell – Free Essay Samples
“Animal Farm” by George Orwell is a literary masterpiece that tells the story of a group of farm animals who rebel against their human farmer and establish a socialist community based on the principles of equality and mutual respect (Orwell, 1945). However, over time, the pigs who lead the revolution gradually become corrupted by power and begin to oppress and exploit the other animals, ultimately turning the farm into a totalitarian state.

Essay on Cyberbullying – Free Essay Samples
Bullying is an aggressive behavior that is intentional and repeated, aimed at causing harm or discomfort to a person, and often takes place in social environments such as schools, workplaces, and online platforms. Cyberbullying is a relatively new form of bullying that has emerged with the widespread use of technology and the internet. Cyberbullying refers to bullying behaviors that occur online or through electronic means, such as social media, text messages, and emails.

Essay on Nature vs. Nurture – Free Essay Samples
The debate over nature versus nurture has been a longstanding topic of interest among psychologists and other scholars. The two concepts, nature and nurture, are frequently used to explain human development and behavior.

Lord of the Flies Essay – Free Essay Samples
Veterans have played a critical role in the history of the United States, serving their country in times of war and peace. Despite their sacrifices, many veterans face significant challenges, including physical and mental health issues, homelessness, and unemployment.

Why Veterans Are Important – Free Essay Samples
Veterans have played a critical role in the history of the United States, serving their country in times of war and peace. Despite their sacrifices, many veterans face significant challenges, including physical and mental health issues, homelessness, and unemployment.

American Dream Essay – Free Essay Samples
The American Dream has been a central concept in American culture for decades, representing the idea that anyone, regardless of their background, can achieve success and prosperity through hard work and determination. The concept of the American Dream is rooted in the country’s history and has been promoted in various ways, from the founding fathers’ beliefs to the post-World War II era.